La variolle simienne : Ce que nous savonsLa viruela del mono: Lo que sabemos猴痘:我们已掌握的情况Monkeypox: Ano Ang Alam Naminਮੰਕੀਪੌਕਸ (Monkeypox): ਅਸੀਂ ਕੀ ਜਾਣਦੇ ਹਾਂBệnh đậu mùa khỉ: Những Điều Chúng Ta Cần Biếtجدري القرود: ما نعرفه عن المرضLast updated: April 15, 2024 The monkeypox virus (MPX/MPOX) has been circulating in Ontario since 2022 […]
MPOX: What We Know

- News
- >
- MPOX: What We Know
MPOX: What We Know
March 20, 2024
Last updated: April 4, 2024
The monkeypox virus (MPX/MPOX) has been circulating in Ontario and around the world and has mostly been reported among gay and bisexual men, passing through close personal and sexual networks.
We have compiled information from public health authorities—including Toronto Public Health, Public Health Ontario, and the office of the Chief Medical Officer of Health—along with relevant news reports and published scientific research. The information on this page is meant to help people in our community understand what’s going on, what to look for, and where to get care. We’re keeping an eye out for reliable sources and updating this page regularly.
Vaccine Information
IS THERE A VACCINE?
There’s no specific MPOX vaccine, but it looks like the smallpox vaccine is about 75%-85% effective at preventing infection and serious symptoms. The last countries stopped giving smallpox vaccines about 40 years ago, so anyone older than 40 might have received it. Even for people who were vaccinated with the smallpox vaccine as children, there is benefit in getting the newer vaccine if you meet the eligibility criteria.
Getting the vaccine early to help prevent MPOX is known as pre-exposure prophylaxis (PrEP). If you have close contact with someone with a confirmed case of MPOX, but don’t have any symptoms, then getting the vaccine is known as post-exposure prophylaxis (PEP). This is similar to how HIV PrEP and PEP work.
IS THE VACCINE SAFE?
Yes, the vaccine that is being used in Ontario (called Imvamune) is safe. It is authorized for use in Canada in people 18 years and older and is delivered by injection into the arm. You can receive the vaccine regardless of when or whether you were vaccinated for COVID-19.
According to the Public Health Agency of Canada, Imvamune’s safety has been assessed in 20 completed clinical trials where approximately 13,700 vaccine doses were given to 7,414 individuals.
In Canada, each vaccine dose gets inspected before it is administered to make sure it is not expired and that nothing has happened to it during storage or transportation. In one instance in Ottawa, for example, some doses in a batch of Imvamune vaccines didn’t look exactly like others, and so local public health officials made the call to not administer any doses from that batch, just to be safe.
HOW SOON AFTER GETTING THE VACCINE WILL IT BE EFFECTIVE?
It takes up to 14 days from the time you get the vaccine to have adequate protection.
VACCINATION CLINICS
Getting vaccinated against MPOX can help reduce your chances of getting it and reduce serious symptoms if you get it.
Remember: vaccines don’t work like an on/off switch. It can take two weeks for your body to process and react to the vaccine after getting it.
The Ontario government takes care of making vaccines available across the province. Local public health units take care of setting up vaccine clinics and actually giving people the vaccines. This section will be updated as we get info from the health authorities.
Toronto Vaccine Clinics
Dundas W. at Bloor St. W
2340 Dundas St W
Toronto, ON
M6P 4A9
Mondays to Thursdays
Various Daytime Hours
Near Ellesmere Rd. and Brimley Rd.
160 Borough Drive
Scarborough Civic Centre
Toronto ON M1P 4N8
Mondays to Thursdays
Various Daytime Hours
27 Roncesvalles Ave.
Suite 505
Toronto
2nd Location:
26 DALHOUSIE STREET (GROUND)
TORONTO, ONTARIO
By appointment only. Call 647-657-4033 to check availability and to book. For more information about the Safer Six clinic, visit SaferSix.ca.
Drop-ins and booked appointments are now available at all six City of Toronto immunization clinic locations.
You can book your appointment through the Toronto Public Health Appointment Booking System.
For more information about the City of Toronto’s vaccine clinics, visit:
Ottawa Vaccine Clinics
420 Cooper St.
Ottawa
Appointments are being offered over the next several weeks. You can call (613-580-6744) or check online for the next available spots.
179 Clarence St.
Ottawa
For more information about the City of Ottawa’s vaccine clinics, visit:
ottawapublichealth.ca/en/public-health-topics/monkeypox-virus.aspx
Simcoe Muskoka District Health Unit Vaccine Clinics
Simcoe Muskoka District Health Unit
15 Sperling Dr.
Barrie
By appointment only
For more information speak with a public health professional at 705-721-7520 or 1-877-721-7520
Durham Region Vaccine Clinics
Oshawa Sexual Health Clinic
419 King St W., Suite 180
West side mall entrance
Lower level
Oshawa
By appointment only. Call 905-433-8901 or 1-800-314-8533 to book. For more information on Durham Region vaccine clinics, visit:
Pickering Sexual Health Clinic
1355 Kingston Rd., Unit 14A
Lower Level
Pickering
By appointment only. Call 905-420-8781 to book. For more information on Durham Region vaccine clinics, visit:
The Positive Care Clinic
Lakeridge Health Whitby
300 Gordon St.
Whitby
By appointment only. Call 905-668-6831 ext. 53127 to book. For more information on Durham Region vaccine clinics, visit:
To book an appointment and find more information about the Durham Region vaccine clinics, visit:
Halton Region Vaccine Clinics
Oakville Sexual Health Clinic
Health @ 232
232 South Service Rd., Unit B
Oakville
By appointment only. Call 3-1-1 or 905-825-6000 to book.
For more information on Halton Region Public Health vaccine clinics, visit:
www.halton.ca/For-Residents/Immunizations-Preventable-Disease/Diseases-Infections/Monkeypox
Middlesex—London Region Vaccine Clinics
MLHU Citi Plaza
Training Rooms, 1st Floor
110-355 Wellington St.
London
Appointments available on select Mondays and Wednesday
evenings.
To book your appointment, please call 226-289-3560.
For more information https://www.healthunit.com/monkeypox
Niagara Region Vaccine Clinics
Mpox vaccines are available at Niagara Region Public Health clinics by appointment. Call 905-688-8248 ext. 7425 or 1-800-263-7248 to book.
For a list of clinic locations and other information, visit:
www.niagararegion.ca/health/vaccinations/
general/default.aspx
For more information on mpox from Niagara Public Health, visit:
www.niagararegion.ca/health/infectious-diseases/mpox/default.aspx
Timiskaming Region Vaccine Clinics
Timiskaming Health Unit Office
247 Whitewood Ave.
Unit 43
New Liskeard
By appointment only. Get upcoming availability and book your appointment by calling 705-647-4305 or 1-866-747-4305.
Timiskaming Health Unit Office
31 Station Rd. North
Kirkland Lake
By appointment only. Get upcoming availability and book your appointment by calling 705-567-9355 or 1-866-866-747-4305..
Timiskaming Health Unit Office
63 Fifth St.
Englehart
By appointment only. Get upcoming availability and book your appointment by calling 705-544-2221 or 1-866-544-2221.
Thunder Bay Vaccine Clinics
By appointment only. Get upcoming availability and book your appointment by calling 807-625-5900 (toll-free: 1-888-294-6630). Ask to speak with the Vaccine Preventable Diseases program.
York Region Vaccine Clinics
17150 Yonge St.
Newmarket
By appointment and walk-in. Visit york.ca/monkeypox to book an appointment.
50 High Tech Rd.
Richmond Hill
By appointment and walk-in. Visit york.ca/monkeypox to book an appointment.
9060 Jane St.
Vaughan
By appointment and walk-in. Visit york.ca/monkeypox to book an appointment.
Brant County Vaccine Clinics
To book an appointment on Monday-Friday, 9AM-4PM please call the sexual health program at 519-753-4937 ext. 471
Elgin and Oxford Vaccine Clinics
1230 Talbot St.
St. Thomas
By appointment. Call 1-800-922-0096 x 1278 to book.
410 Buller St.
Woodstock
By appointment. Call 1-800-922-0096 and follow the prompts to speak with the Sexual Health team to book.
Haliburton, Kawartha, and Pine Ridge Vaccine Clinics
HKPRD Health Unit Office
108 Angeline St. South
Lindsay
By appointment only. Call 1-866-888-4577, ext. 1507 to book. For more information on HKPRD Health Unit vaccine clinics, visit:
HKPRD Health Unit Office
200 Rose Glen Rd.
Port Hope
By appointment only. Call 1-866-888-4577, ext. 1507 to book. For more information on HKPRD Health Unit vaccine clinics, visit:
Hamilton Vaccine Clinics
David Braley Health Sciences Centre
100 Main St. West, 3rd Floor
Hamilton
Hours of Operation: Wednesdays 4.30 pm to 7.30 pm
By appointment only. Call 905-528-5894 to book. For more information on Hamilton vaccine clinics, visit:
Kingston Vaccine Clinics
221 Portsmouth Ave.
Kingston
By appointment only. For more information on KFL&A Health Unit vaccine clinics and to book an appointment, visit:
844 Princess St.
Kingston
By appointment only. For more information on KFL&A Health Unit vaccine clinics and to book an appointment, visit:
For more information on KFL&A Health Unit vaccine clinics and to book an appointment, visit:
Northwestern Region Vaccine Clinics
Northwestern Health Unit Office
75-D Van Horne Ave.
Dryden
By appointment only. Get upcoming availability and book your appointment by calling 1-800-830-5978.
For more information on Northwestern Health Unit vaccine availability, visit:
Peel Region Vaccine Clinics
Fairview Clinic
325 Central Parkway West
Mississauga
By appointment only. Call 905-799-7700 to book.
Brampton Clinic
150 Central Park Dr.
Brampton
By appointment only. Call 905-799-7700 to book.
Sudbury Region Vaccine Clinics
Public Health Office
1300 Paris St.
Sudbury
By appointment only. Get upcoming availability and book your appointment by calling 705-522-9200 x 482 (toll-free: 1-866-522-9200).
For more information on Public Health Sudbury & Districts vaccine clinics, visit:
Réseau ACCESS Network
111 Larch St., Unit 101
Sudbury
By appointment only. Get upcoming availability and book your appointment by calling 705-688-0500.
For more information on Public Health Sudbury & Districts vaccine clinics, visit:
Waterloo Region Vaccine Clinics
Region of Waterloo Public Health Office
150 Main St.
Cambridge
By appointment only. See upcoming availability and book your appointment online or call 519-575-4400.
For more information on Region of Waterloo Public Health vaccine clinics and to book an appointment, visit:
regionofwaterloo.ca/en/health-and-wellness/infectious-disease.aspx#Monkeypox
Region of Waterloo Public Health Office
99 Regina St. S
Waterloo
By appointment only. See upcoming availability and book your appointment online or call 519-575-4400.
For more information on Region of Waterloo Public Health vaccine clinics and to book an appointment, visit:
regionofwaterloo.ca/en/health-and-wellness/infectious-disease.aspx#Monkeypox
Windsor Region Vaccine Clinics
Windsor—Essex County Health Unit
1005 Ouellette Ave.
Windsor
By appointment only. Get upcoming availability and book your appointment by calling 519-258-2146 ext. 1420.
For more information on Windsor—Essex County Health Unit vaccine clinics, visit:
ONTARIO PUBLIC HEALTH UNIT LOCATOR:
To find your local public health unit, click here:
If you don’t see your community in this list, please contact your local public health unit or call the Sexual Health Infoline Ontario (SHILO). SHILO is a free, province-wide anonymous counselling service on HIV, STIs, safer sex, referrals to sexual health services, testing information, harm reduction in drug use, and needle exchange information.
416-392-2437 / 1-800-668-2437 (English and multilingual Line)
You will not be asked to pay for the vaccine. You do not need an OHIP card to get the vaccine.
Note: The GMSH is sharing this information to support our community and to promote vaccination for those of us who may benefit from it. We aren’t responsible for running any of the clinics, how many doses are available, or the individual experience of people at the various vaccine clinics that are set up across the province.
Who should get the vaccine?
You should consider getting vaccinated against MPOX (Imvamune, the smallpox vaccine) if you have had an STI in the last few months, if you have sex with multiple partners, if you have anonymous sex, if you go to places where sex happens (like the bathhouse), or if you do sex work.
The current eligibility criteria determined by the Ontario Ministry of Health are:
a) Two-spirit, non-binary, transgender cisgender, intersex, or gender-queer individuals who self-identify or have sexual partners who self-identify as belonging to the gay, bisexual, pansexual and other men who have sex with men (gbMSM) community AND at least one of the following:
- Had a confirmed sexually transmitted infection within the last year;
- Have or are planning to have two or more sexual partners or are in a relationship where at least one of the partners may have other sexual partners;
- Have attended venues for sexual contact (e.g., bath houses, sex clubs) recently or may be planning to, or who work/volunteer in these settings;
- Have had anonymous sex (e.g., using hookup apps) recently or may be planning to; and/or
- Are a sexual contact of an individual who engages in sex work.
b) Individuals who self-identify as engaging in sex work or are planning to, regardless of self-identified sex or gender.
c) Household and/or sexual contacts of those identified for PrEP eligibility in parts (a) and (b) above AND are moderately to severely immunocompromised or pregnant may be at higher risk for severe illness from an MPX infection may be considered for PrEP and should contact their healthcare provider (or their local public health unit) for more information.
The vaccine being used, Imvamune, is meant to be given as a single dose initially and then as a second dose at least 28 days later.
There’s no evidence that waiting longer than 28 days to get the second dose changes how effective the first dose is. Generally, waiting longer between first and second doses of any vaccine leads to a better immune response. And while two is better than one, one is still better than none.
You can get the second dose of the vaccine at least 28 days after getting your first dose. Check the vaccine section above for details or call your local public health unit to book an appointment.
In Canada, all Imvamune vaccines are being given in full doses.
Sometimes, a vaccine can be administered as a partial dose (known as fractional dosing), where only 20% of the volume of a single dose is administered. There’s some evidence that this can be as effective as a full dose, and some evidence that it has a higher chance of causing side effects from the vaccine.
Authorities in the United States have approved fractional dosing in order to reach more people, given their extremely limited supply of vaccines. In Canada, there has so far been no vaccine shortage for the target population, and so public health officials haven’t used fractional dosing.
In Canada, this vaccine is purchased and managed by the federal government through the National Emergency Stockpile. The federal government, informed by the National Advisory Committee on Immunization (NACI), establishes general strategies for how the vaccine will be used in this outbreak response.
Both the guidelines and the vaccines themselves are then handed off to each provincial or territorial government. These governments are responsible for refining the eligibility criteria for their specific region and for coordinating implementation. The rules for eligibility and administration set out by the provincial government are applied equally across the province.
These rules and the vaccine doses then get handed off to local Public Health Units (PHUs). The PHU is responsible for setting up immunization clinics, training nurses, and administering the vaccine doses.
The vaccine being used against MPOX, called Imvamune, is a specialized vaccine that was developed for people who couldn’t have earlier generations of the smallpox vaccines. Because countries no longer vaccinate the general population against smallpox, there was very low demand for this product and only one manufacturer.
At the start of this outbreak, Canada was already in a very good position, with doses of Imvamune available in the National Emergency Stockpile. That meant that we were the first country to roll out a large, targeted vaccination campaign to help slow the spread of the virus.
So far, there has been no issue getting at least a single dose to everyone who is at high risk of being exposed to monkeypox in Ontario, and second doses for those who are immunocompromised.
We have heard that the federal government has ordered more doses from the manufacturer, but that those will not arrive until 2023.
MPOX: The Basics
It’s a virus that can cause a rash, lesions, or blisters, along with fever, muscle aches, and extreme tiredness. Both animals and humans can contract the virus, and it’s spread by close and prolonged contact. It’s in the same family as smallpox, but MPOX is less contagious and has milder symptoms.
Historically, most cases were reported in central and western African countries. Before this year, it was very rare to see cases in Canada or the US.
Symptoms typically show up within about five days of exposure to MPOX, but can take up to 21 days to show up. They can include:
- A rash or blisters in your mouth (like a canker sore), on your face, around your genitals, or around or in your butt
- Swollen lymph nodes
- Fever and chills
- Muscle aches
- Headaches
- Exhaustion
Very serious symptoms are possible but are less common. Recently, between 3%-6% of cases have led to death.
In this most recent outbreak, some people had the rash or blisters appear first before feeling tired and feverish. And in some cases, people didn’t have any noticeable symptoms.
-
Photos of MPOX Lesions (Graphic):
These photos were taken of people with confirmed cases of MPOX in the UK, Italy, and Australia in May 2022.
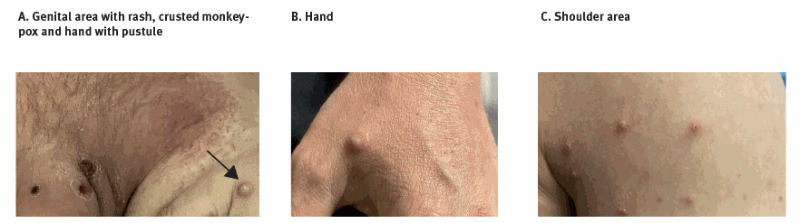
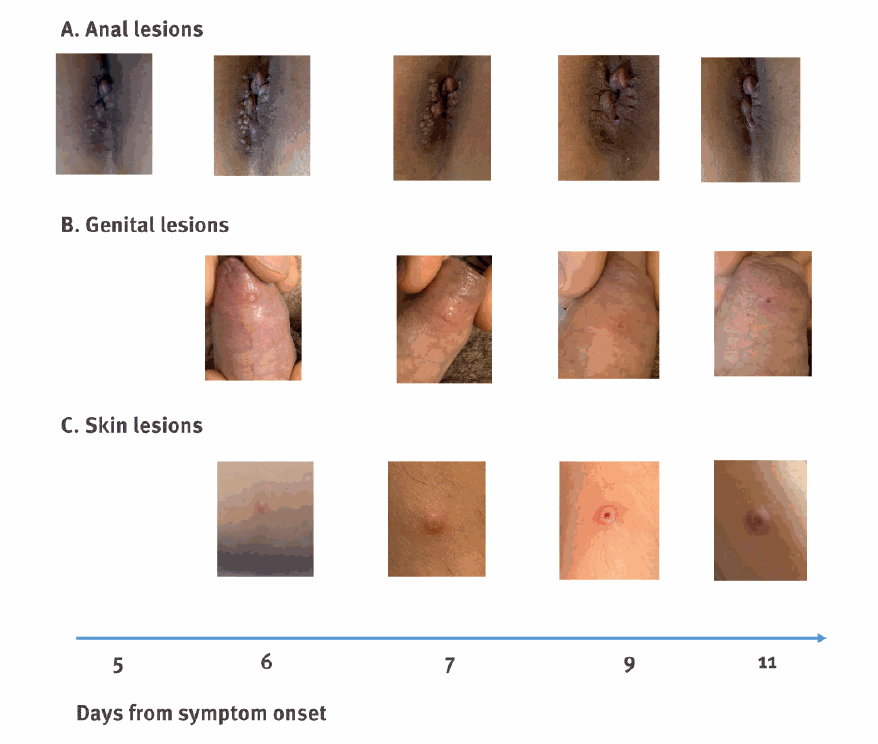
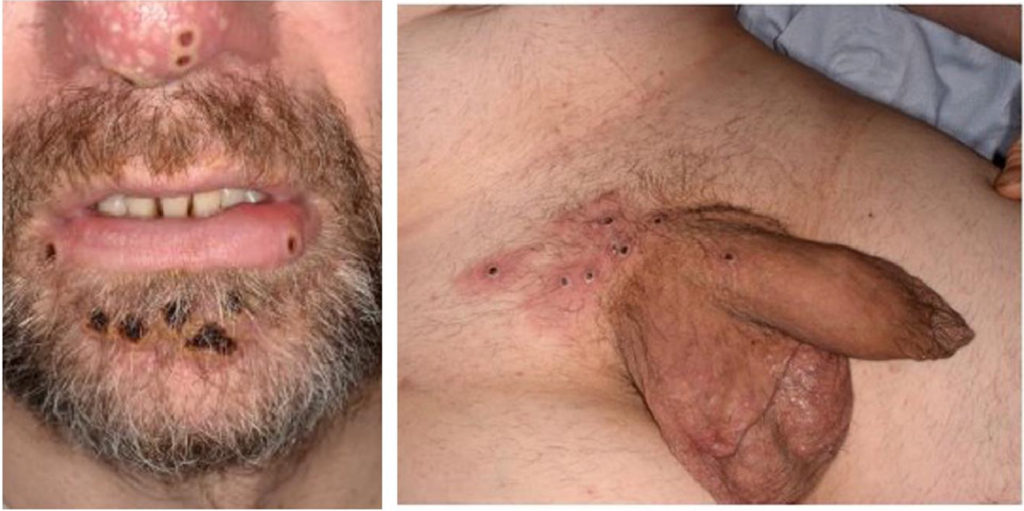
MPOX lesions on the face and at the base of the penis.
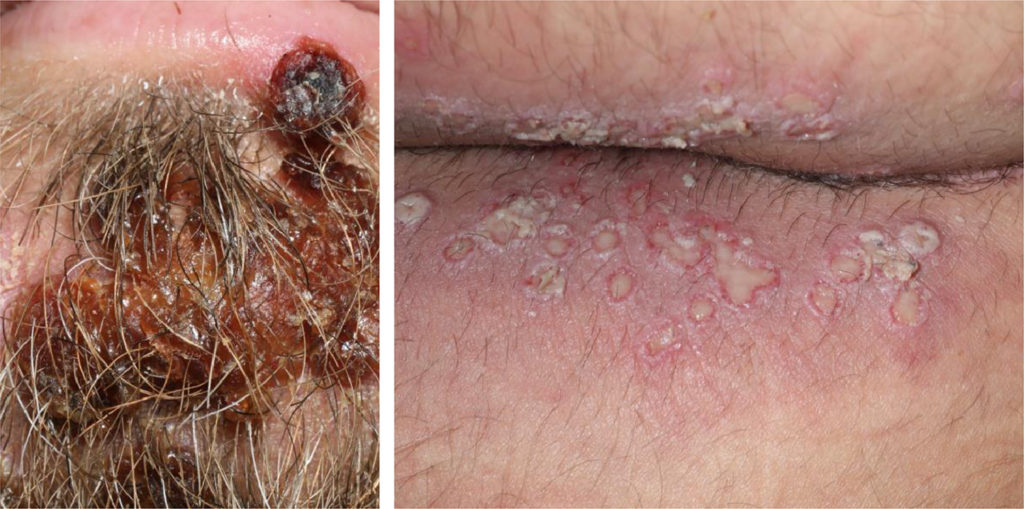
MPOX lesions around the mouth and around the ass.
The full reports on these cases are available at the bottom of this page.
Transmission
The MPOX virus can be transmitted by respiratory droplets, by touching a lesion or blister, or contaminated surfaces like clothes or bedding.
It typically needs prolonged face-to-face or body contact to spread. That means it doesn’t tend to spread very quickly or very far.
So far, it seems like the current outbreak is mostly linked to extended skin-to-skin contact, sex, kissing, or very close talking. It seems very unlikely that it’s been passed along just by being in the same space as someone else, a handshake or hug, or walking by another person.
It is possible to pass on the virus in the days before you have any noticeable symptoms.
Yes, you can get MPOX from sexual contact. We know that it’s transmitted through close contact like hugging, kissing, humping, or cuddling. So if you’re close enough to have sex, there’s a chance of getting it or passing it along.
BUT! That doesn’t mean that you can only get it from sex. There are some cases in the current outbreak where nothing sexual happened, and in places where this virus is endemic, transmission is very rarely linked to sexual contact.
So does that mean it is or it isn’t an STI? As far as we’re concerned, that label doesn’t make a difference for how most gay men are living our lives.
We know that the virus is moving through close personal and sexual networks, and that the vast majority of cases in Ontario are linked to intimate contact.
Yes, wearing a condom may help, if someone has spots on their dick or in their ass. But given that the virus can be passed on through saliva and skin-to-skin contact, a condom alone isn’t a guarantee.
That said, the virus has been detected in semen even after other symptoms have cleared up. In Canada, it is recommended to wear a condom for at least 12 weeks after all symptoms have cleared. This would probably only be effective if you used a condom the entire time you had sex, including when giving or getting head, and didn’t get cum anywhere other than in the condom.
Testing
If you spot a new rash or blisters or any of the other MPOX symptoms, contact your healthcare provider right away. If you don’t have one, the next best option is your local sexual health clinic. If that’s not an option, then you can call either your local public health unit or the Sexual Health Infoline Ontario (SHILO).
You should get tested as soon as possible. Anywhere in Ontario that can test for a virus like syphilis can also test for MPOX. If your healthcare provider isn’t sure about it, share this guidance with them:
publichealthontario.ca/en/Laboratory-Services/Test-Information-Index/Monkeypox-Virus.
In the meantime, keep any lesions covered, wear a mask if you’re around and close to other people, and avoid close contact as much as you can until you get your test results back. It’s also a good idea to write down notes on things like when you first noticed symptoms and any changes in symptoms.
It’s going to be ok. Remember that MPOX is time-limited and you will recover. Based on current data, relatively few people have had severe complications or passed away in the current outbreak, out of 85,000 plus cases worldwide.
Having MPoX can really range in terms of symptoms. Some guys have no obvious symptoms, with either no or a small handful of lesions, while others can have 20+, a rash, fever, and swollen lymph nodes. The pain you have will likely depend on where the lesions are located, with the inside of your ass, urethra, and mouth being at the top of the list, followed by lesions around your ass and on or around your genitals. Lesions on your hands and feet can be a real pain because of the pressure applied when we move around.
Treatment and Care
As with any infection, your body and immune system are in overdrive working to overcome it.
Don’t forget the basics:
- Rest and stay hydrated.
- Take your regular medications at the usual time unless advised otherwise .
- Wash your hands frequently and especially after caring for lesions.
This might be the most uncomfortable part of your day. You’ll be advised to keep lesions covered and told that when the lesions clear up, you are considered recovered from MPOX, meaning no more isolation.
To promote healing and prevent scarring:
- Apply Vaseline on the lesion and cover it as soon as it appears (when small like a zit) – other topical creams may reduce pain but be sure to consult with a healthcare provider first.
- Keep covered with a bandage to promote fast healing – guys with MPOX are sharing tips and tricks on the best dressings to use.
- Avoid scratching or picking the lesions.
- Be aware of fabrics touching your skin.
Many people with MPOX have uncomfortable symptoms like swollen lymph nodes (especially in the groin area), fever, and feeling unwell.
- For pain when taking a shit, using stool softeners might be helpful, mainly because the inside of your rectum will be swollen. This is called proctitis.
- If you experience significant bleeding or bleeding that won’t stop from any part of your body, call your doctor or visit your local emergency department.
Unfortunately, because this current outbreak is new and the way it’s getting passed along isn’t typical, it’s hard to find solid medical guidance on caring for yourself. But gay men have a history of taking care of ourselves and each other, and many gay physicians and guys with MPOX have been sharing what works for them.
Some of the more common suggestions include:
- Sitz baths can provide comfort from lesion pain – especially for your butt and genitals.
- Salt gargle for lesions in your mouth.
- Topical steroids.
- OTC pain meds like acetaminophen (Tylenol) and ibuprofen (Advil) for aches and pains.
- Gabapentin (a medication used to treat pain from shingles) and opioids, if the pain is really bad. These would need to be prescribed by a doctor.
A diagnosis of MPOX means isolating at home for an extended period (sometimes as long as a month), avoiding close contact with family and roommates if living together, any pets, avoiding sexual contact, and missing work or school, unless you can do it from home. Remember the COVID-19 lockdowns—think about what helped you get through that period. Zoom rooms, movie watching days, catching up on a good book. Do things that make you feel good and lean on the people in your life as much as you can.
Guys have taken it upon themselves to host supportive spaces for people with MPOX – these are not always formal like therapy but offer a chance to share experiences and hear from others.
There’s not a ton of support available for people, especially financial support to make up for any lost income due to isolation. When diagnosed, be sure to ask the clinic staff or public health professionals about any help they can provide. Sometimes this includes things like grocery cards to get food delivered to you.
In Ontario, we are aware of the following:
- Ontario Works helps people who are in temporary financial need. It includes Emergency Assistance for Ontarians who are in a crisis or facing an unexpected emergency and are unable to meet basic living expenses.
- Emergency Assistance may be provided for 48 days. A complete application for income assistance is required to continue assistance beyond 48 days.
- Eligible individuals may receive approximately $733 a month if they are a single person and need help paying for food and shelter. They may receive more if they have children.
- People can apply for emergency assistance either in person at a local Ontario Works office, OR they can apply online.
- Ontario Works Administrators determine eligibility for emergency assistance based on an assessment of the applicant’s ability to access other resources and meet their basic living expenses and the danger to health or risk that a child would be unable to continue living with the family if assistance is not issued.
- People already receiving Ontario Works or ODSP are not eligible for emergency assistance. Tourists and visitors are also not eligible.
For more on how to care for yourself while recovering from MPOX, check out this graphic by the World Health Organization (WHO). For a first-hand account of what it’s like to have MPOX and tips on lesion care, and more from someone experiencing it check out IGotMpox.com.
MPOX and the Party
We know that the party doesn’t stop after Pride. Across Ontario, our community is coming together to experience the joy (and sex!) that Pride, festivals, and parties offer.
Here are some things to be aware of and some things we can all do to take care of our sexual health and of our community.
Get vaccinated, if you can. It can help stop infection and serious symptoms.
Visit your family doctor or local sexual health clinic and get a full screening for sexually transmitted infections (including syphilis and HIV). Remember to ask for swabs alongside the other tests. For a lot of us, testing includes our throat and asshole in addition to peeing in a cup and having our blood taken.
- Check around your ass and genitals for any new bumps, lumps, rashes or anything else that might look unusual for you.
- If you notice anything, schedule a visit with your healthcare provider
- You might need to remind them that MPOX is going around the community.
- If you develop symptoms of MPOX, consider isolating and avoiding close contact—including sex— until you have been assessed by a healthcare provider and they have ruled out MPOX.
- Consider how much close contact (kissing, skin contact, sex) you’re going to have with people at parties, places, and other venues before you go.
- Continue to take your PrEP or HIV medications as prescribed.
- Keep condoms and lube on hand. There’s a chance that MPOX can be transmitted through cum, but condoms are still helpful at preventing other STIs.
- Think about limiting the number of partners you have or going to events or venues with a lot of close contact.
- If you can, having some basic contact info for the people you have sex with or get close to—whether at venues or on hook-up apps—can be helpful if you need to contact them for potential MPOX exposure.
- Other ways you can reduce the risk of MPOX:
- Avoid sharing—lube, sex toys, fetish gear, douching equipment, toothbrushes, substance use equipment like pipes and syringes, bedding, towels and clothing.
- If sharing, try to use barriers like gloves for fisting and condoms on sex toys. Change them out between sex partners.
- The more sexual partners you have, the higher chance that you might be exposed to MPOX or pass it on.
- Avoid sharing—lube, sex toys, fetish gear, douching equipment, toothbrushes, substance use equipment like pipes and syringes, bedding, towels and clothing.
- Talk openly with your partners about your sexual health and theirs—we all want to have a good time, and it’s up to all of us to care for each other.
- Monitor for any symptoms of MPOX including any new bumps, lumps, rashes, or anything else that might look unusual for you.
- Follow the guidance of your doctor, sexual health clinic staff, or other healthcare provider.
- You might need to remind them that MPOX is going around the community.
- Visit your family doctor or local sexual health clinic and get a full screening for sexually transmitted infections (including syphilis and HIV). Remember to ask for swabs. For a lot of us, testing includes our throat and asshole in addition to peeing in a cup and having our blood taken.
-
How serious is MPOX?
MPOX is a serious disease. While many people who get MPOX won't have really bad symptoms, lots of people in the current outbreak are. Some (but not most) people have ended up in the hospital, and people who have had more serious symptoms reported severe pain; blisters and open sores in their mouth, on their face, ass, or dick; and—in some cases—bleeding from the sores or blisters they had (including from their ass). Treatment is available for anyone hospitalized who is severely ill.
From the case reports that have been made public in the current outbreak, we know that people with MPOX can experience a range of symptoms with varying degrees of pain and discomfort. Depending on how well the lesions heal, scarring is possible.
-
Is the vaccine safe for people living with HIV?
People living with HIV who take HIV treatment have less sever experiences with MPOX. People living with HIV who have a CD4 count of less than 100, have persistent high viral load, or are otherwise immunocompromised may experience more severe illness and should talk to their healthcare provider before getting the vaccine.
The vaccine that you will be offered is safe and studies included people living with HIV. You may be asked about your CD4 count. Regardless, if offered the vaccine you should consider taking it for the protection and benefits it offers.
-
What are the vaccine side effects?
Imvamune, the vaccine available in Canada, is being given as a single needle injection. It’s injected on the underside of your arm, just under the skin.
Most people don’t have a strong reaction to the vaccine. The most common side effects are feeling sore, some light bruising, a small bump, swelling, or a small rash around where you get the needle.
Some people feel tired, get headaches or muscle pain, and occasionally feel sick to their stomach. If you do experience these, they typically go away within a week. The injection shouldn’t leave a scar.
If you do have a strong reaction, or if the side effects last longer than a week, get in touch with your healthcare provider or local public health unit.
-
Is it just affecting queer men?
So far, reports are that it’s mostly passing through some sexual networks among men who have sex with each other, but there's no clear connection between most of the confirmed cases. There are some cases that don’t involve gay or bisexual men, too. The virus doesn’t target people and so any prolonged contact (not necessarily sexual) can pass it along. Plus, it can live in animals, which has caused outbreaks in the past (most recently in 2003 in the US).
-
MPOX and HIV
Like many infections, the impact of MPOX can be worse for people with weakened immune systems. For people living with HIV who aren’t on treatment or have low T-cell counts, it is possible for more complications to come up if they contract MPOX. There’s no evidence that someone living with HIV who is undetectable has any greater risk of complications from MPOX than someone without HIV.
-
How concerned should you be?
Don’t panic, but you should be aware. Being alert and telling your doctor or local public health unit about any symptoms you have can help slow its spread.
Even if you might have a mild case, there are people in our community with compromised immune systems who could get seriously sick.
If you see a report of MPOX linked to a particular place (like a club, bar, or bathhouse) that you were at, think about what you did there and if you had any close contact with people.
Public Health Units in Ontario are doing contact tracing for the possible cases in the province and following up directly. But for the next while, it is probably best for everyone to keep track of who they have been in close contact with (ex. kissed, had sex with, or been naked with) and be proactive about reaching out to them if you develop symptoms or have a confirmed case. Same goes for any venues you were in over the last three weeks, if you kissed, shared drinks with, or had sex with someone else who you can’t contact directly.
-
Duty to report
In Ontario, the Chief Medical Officer of Health has ordered all healthcare providers to report any suspected or confirmed cases of MPOX to the CMOH and to Public Health Ontario.
For more information:
https://www.who.int/news-room/fact-sheets/detail/monkeypox
https://www.cdc.gov/poxvirus/monkeypox/index.html
https://www.health.gov.on.ca/en/pro/programs/emb/monkeypox.aspx
https://www.quebec.ca/en/health/health-issues/a-z/monkeypox
https://www.canada.ca/en/public-health/services/diseases/monkeypox.html
https://www.catie.ca/catie-news/an-outbreak-of-monkeypox-in-canada-and-other-countries
https://www.eurosurveillance.org/content/10.2807/1560-7917.ES.2022.27.22.2200411
https://www.eurosurveillance.org/content/10.2807/1560-7917.ES.2022.27.22.2200421
https://www.journalofinfection.com/article/S0163-4453(22)00335-8/fulltext
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2168110/
https://www.cdc.gov/poxvirus/monkeypox/clinicians/smallpox-vaccine.html